Table of Contents
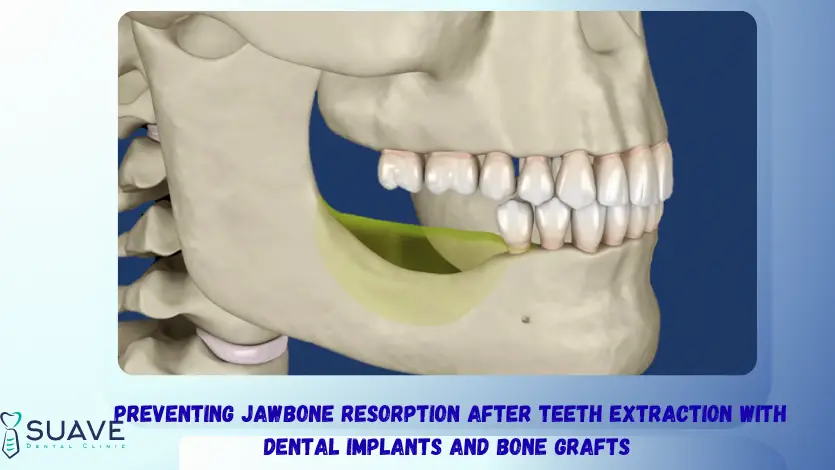
Did you know that after a tooth extraction, alveolar bone loss of up to 25% bone volume or width can occur within the first year, and upto 40%-60% in the second year, if no treatment is performed?
Jawbone resorption doesn’t happen suddenly; it develops silently as a result of a series of factors that may go unnoticed, including prolonged tooth loss, chronic gum disease, or even certain underlying medical conditions.
The jaw consists of two plates of bone; Alveolar bone which is an essential part of the periodontium (gingiva and bone tissues supporting and surrounding the teeth) covered by the gingiva, and the most affected part by teeth extraction, the second part is the basal bone, which is compact bone of the jaw at the lower part of the skull that certain face muscles attach to, and doesn’t relate to the supporting tissues of the teeth.
Alveolar bone resorption happens when the balance between bone breakdown and new bone formation (bone remodeling process) shifts more towards breakdown as a result of some inducing factors.
Causes of the resorption of the jawbones
Early awareness of the causes of jawbone resorption is the first step in maintaining oral health and avoiding complex treatment later on. Here are the main ones:
- Neglecting or delaying the replacement of missing teeth
When a tooth is extracted or missing for a long time without replacement or restoration, the surrounding jawbone stops receiving stimulation from chewing food, leading to bone volume shrinkage (bone atrophy), which is very common as a complication of tooth extractions.
- Using an ill-fitted removable denture
An ill-fitted removable denture or prosthesis resting on the gingiva, applying uneven pressure to the underlying bone, compressing the blood supply to the alveolar bone, and causing jawbone loss over time, unlike implant-supported overdentures, all-on-4, or all-on-6 dental implants. - Longstanding gum diseases
Untreated gingivitis and periodontitis, which is inflammation of the gum and the surrounding supporting tissues, can lead to inflammation and infection of the bone supporting the teeth. - Trauma or injury to the face or jawbone
Trauma directly damages the jawbone, leading to localized bone resorption, osteonecrosis (bone tissue death), or osteomyelitis (infection). - Misaligned teeth
Misaligned teeth cause uneven biting forces, creating areas of under-stimulation and other areas of “traumatic” overstimulation that trigger bone resorption, like crooked teeth.
Also, misaligned crooked teeth create traps of plaque and bacterial accumulation that are impossible to brush away, which initiates periodontitis and can lead to bone resorption. - Impacted teeth
Impacted teeth damage the bone through mechanical pressure, chronic infection of the neighboring tooth roots, and the potential development of cysts. - Aging and Systemic Conditions
Aging and menopause accelerate bone resorption and slow down new bone formation, which is known as osteoporosis.
Some systemic conditions also can speed up bone degeneration, including osteoporosis, uncontrolled diabetes, rheumatoid arthritis, Paget’s disease, hyperparathyroidism, and malignant disease. - Certain medication intake
Bisphosphonates, certain medications in chemotherapy, radiotherapy, and high-dose corticosteroids, induce bone loss and complicate any dental treatment, as they are major risk factors for medication-related osteonecrosis of the jaw. - Low levels of specific nutrients and vitamins
Calcium and vitamin D deficiency disturb bone metabolism, increasing the risk of osteoporosis. As calcium is the primary mineral for bone integrity and density, and Vitamin D enhances calcium absorption by the tissues and regulates its level in the blood. - Smoking tobacco products
Nicotine and other toxic compounds in tobacco products impair bone reمmodeling and delay healing processes while also reducing bone mineral density, which increases susceptibility to fractures and contributes to the development of osteoporosis.
Effects of jaw bone resorptions
Jawbone loss may often go unnoticed, but it leads to serious impacts on overall oral health and functions, starting after tooth loss:
- Sunken ridge at the part of bone resorption
- Gum recession occurs because the gingiva always follows the bone; in the edentulous area, it is pulled down or indented as bone volume decreases.
- Tilting of the neighboring teeth to the edentulous ridge
- Natural teeth are becoming loose due to tilting or the protrusion of opposing teeth from their socket.
- The patient notices bite or chewing problems in the edentulous area.
- Loss of vertical dimension of the face leads to malocclusion
- Shifting the bite to the dentulous areas causes TMJ problems.
Complications of jawbone resorption
Neglection jawbone loss over time without any missing teeth replacement changes in the structure of the mouth; it is the beginning of a series of complications that can affect appearance, function, and overall quality of life. These are the most common complications:
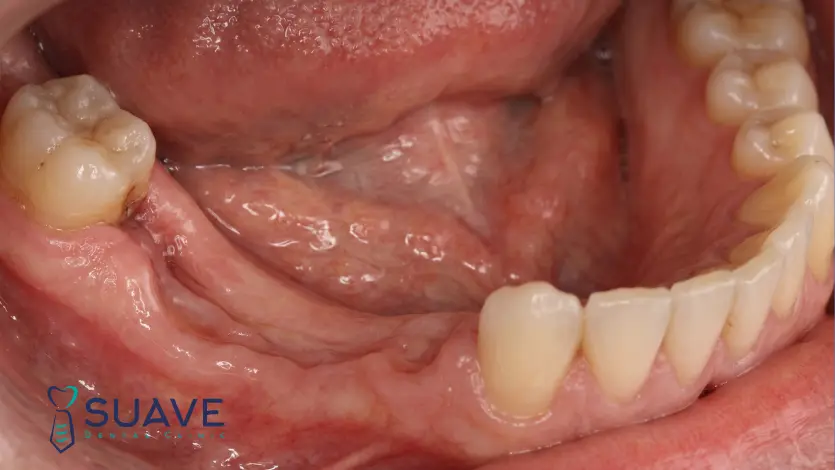
Dental changes due to bone resorption after bone loss:
- Soft tissue inflammation, gingival laceration, and swelling due to chewing food on the gums and the lack of bony support.
- Opposing teeth pain and sensitivity.
- Persistent pain during chewing
- The risk of Oro-antral communication after upper molar teeth extraction, which is an abnormal gap between the maxillary sinus and the oral cavity, resulting from perforation of the thin bony floor as a result of sinus expansion.
Facial changes due to alveolar bone resorption
- Jawbone loss may lead to the lower face shrinking over time, resulting in a “sunken face” appearance.
- Wrinkles around the mouth.
- Thinned lips give an older appearance.
- Facial pain and lower oral functions
- TMJ pain and jaw stiffness
- Jaw fracure incident become very common with any further tooth extraction on the same side
Complications of missing teeth restorations
In advanced bone resorption, there is no proper bone volume for implant placement, and not enough space for dental bridges to restore the missing teeth due to neighboring teeth’s inclination, which leads to surgical intervention in some cases, like:
- Sinus expansion over time leaves inadequate bone space for an upper dental implant in the posterior region.
- Mandibular nerve approximation to the surface of the remaining ridge, which makes any dental implant placement a dangerous procedure with a high risk of nerve puncture and long-lasting numbness.
Dental Treatment of Jawbone Resorption
Jawbone resorption requires an organized, clinically focused strategy to ensure optimal functional and aesthetic outcomes. At Suave Dental Clinic, a variety of advanced treatments are offered and performed based on the extent of bone loss, individual anatomical factors, and overall state of oral health.
- Bone grafting and membrane
Bone grafting procedures can be performed. Using bone from a different area of the body or synthetic grafting materials to restore the jawbone volume and stimulate new bone growth.- Sinus lift surgery
In cases of long-term bone resorption in the upper jaw, which allows sinus pneumatization, sinus lift surgery is needed to elevate the sinus membrane and create space for the bone graft. - Ridge augmentation
Ridge augmentation and bone grafting are more common in the lower jaw, aimed at reconstructing and recontouring the alveolar bone, especially in flabby ridge cases, to enhance both function and aesthetics.
- Sinus lift surgery
- Dental implant for missing teeth replacement
Dental implants are the best solution for restoring tooth loss. They stimulate the jawbone formation and osteointegration through the titanium rod that is implanted in the jawbone, mimicking the natural root of the tooth, which aids in preventing additional bone loss. - Removable Denture Replacement
Poorly fitting dentures may lead to accelerated bone resorption even with frequent denture base relining. Modifying or replacing dentures can relieve pressure on the jawbone and enhance oral function by converting a removable denture into a fixed one, with all-on-4 dental implants or an implant-supported overdenture.
Preventing Jawbone Resorption
Diagnosis in the early stages and addressing the root causes can significantly slow the progression of jawbone loss and keep dental treatment options simpler and more effective
- Keeping good oral hygiene and daily brushing and flossing lowers the incidence of tooth caries, gingivitis, or periodontitis.
- A balanced diet intake, with quitting smoking and alcohol, keeps bone and soft tissue healthy, even with aging
- Early dental treatment for tooth cavities with dental fillings like composite bonding restoration or root canal treatment, avoiding tooth pain and extraction.
- Immediate dental implant placement with a dental crown is the gold standard to replace missing teeth and induce new bone formation, which lowers the risk of bone loss.
- Regular dental check-ups every 3 -6 months and professional cleaning for teeth and gums to keep them healthy, and detect and control any risk factors.
Get A Free Dental Consultation
Get A Personalized Treatment Plan and Quotation
References
Medically Reviewe